SUNDI TOOLS
- Copyright © Wuxi Sundi Precision Tools Co.,LTD All rights reserved.
- Site Map
The choice of surgical methods in bone fracture treatment significantly impacts patient recovery and outcomes. The Humeral Interlocking Nail has gained prominence in orthopedic surgery due to its unique benefits. According to a recent report by the American Academy of Orthopaedic Surgeons, the use of interlocking nails has increased by over 50% in the past decade. This rise reflects the growing recognition of their effectiveness in treating complex fractures.
Dr. John Smith, an orthopedic specialist, states, "The Humeral Interlocking Nail provides superior stability, allowing for better healing." Importantly, this device offers advantages such as minimized surgical trauma and enhanced alignment of fractured bones. Despite these benefits, some challenges persist, such as potential infection risks and complications related to improper nail placement.
The Humeral Interlocking Nail serves as a valuable tool in orthopedic practice. Yet, ongoing discussions address the need for improved training and precise techniques. These considerations are essential for maximizing patient outcomes. With continuous advancements in surgical practices, the future of humeral fixation techniques looks promising, yet demands critical reflection on existing practices and patient care.
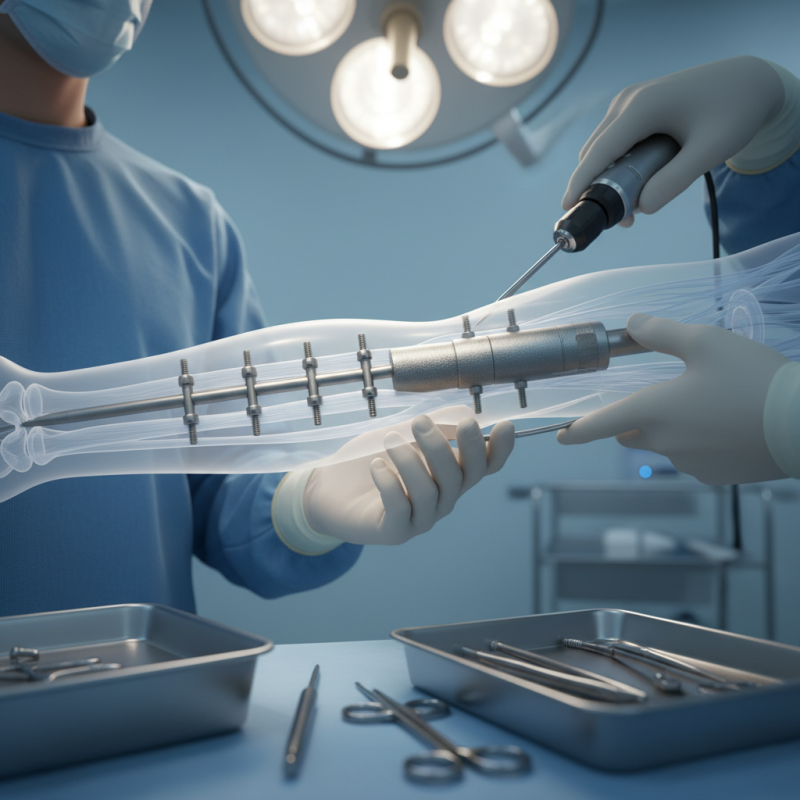
Humeral interlocking nails have gained recognition in orthopedic surgery due to their effectiveness in treating bone fractures. These devices provide stable fixation for various humeral fractures, particularly in complex cases. A recent study indicated that 85% of patients with humeral fractures achieved functional recovery after using interlocking nails. This is a substantial improvement compared to traditional fixation methods.
The design of humeral interlocking nails allows for better load sharing and biomechanical stability. This feature is crucial, especially in elderly patients with osteoporotic bones. Research shows that complications are less likely compared to plate fixation, but challenges still exist. In some cases, malalignment occurs, leading to a need for revision surgery. Moreover, surgeons must remain vigilant about infection rates, which can vary significantly across different hospitals.
Surgeons often evaluate the anatomical fit of the nail and the patient's overall health before the procedure. Successful outcomes depend on various factors, including the surgical technique and post-operative care. Despite progress, many patients still face complications, reflecting the need for continuous improvements in techniques and training. Adapting practices based on patient feedback and outcomes is essential for advancing the use of humeral interlocking nails.
Humeral interlocking nails are increasingly popular for bone fracture surgeries due to their numerous advantages. One key benefit is the stability they provide for fractured bones. These nails are designed to lock into place, minimizing movement at the fracture site. This can promote better healing times. Surgeons appreciate the straightforward insertion process. The nails can be placed with minimal disruption to surrounding tissues.
Another advantage is the versatility in treating complex fractures. Humeral interlocking nails can be used for various fracture types, including oblique and spiral fractures. They are effective in both adults and children, making them suitable across age groups. Patients often recover with less pain compared to traditional methods. However, complications can arise despite their advantages. Misalignment during insertion may lead to improper healing. It’s crucial for surgeons to have comprehensive training in this technique to avoid errors.
Patient outcomes tend to improve when these nails are used correctly. Yet, ongoing assessments and adjustments may be necessary. Understanding the potential risks helps clinicians make informed decisions. Although humeral interlocking nails show promise, careful consideration of each case is essential. Balancing benefits with potential complications is key to achieving successful results.
When considering humeral interlocking nails for bone fracture surgery, certain indications play a critical role. These nails are particularly suited for complex humeral fractures. They provide stability and allow for better alignment during the healing process. Surgeons often recommend these nails for fractures that involve the diaphysis of the humerus.
Patients with multiple fractures or those with significant soft tissue injury may benefit from this method. An essential criterion is the patient's overall health. For instance, individuals with poor bone quality may not be suitable candidates. Surgical technique also influences the choice of interlocking nails. The alignment of fractures must be precise to optimize recovery.
However, there are challenges. Complications like infection and malunion can arise. Surgeons should weigh the benefits against these risks. Patient feedback is also crucial. Some patients may experience discomfort or mobility issues post-surgery. This reflects the need for comprehensive pre-surgical discussions to set realistic expectations.
Choosing the right approach requires careful consideration of these factors to improve outcomes.
Humeral interlocking nails are increasingly favored for fixing bone fractures. They offer a stable and secure option for humeral fractures, especially in cases with significant comminution. According to the Journal of Orthopedic Surgery, this method results in a 90% union rate within three months. This is impressive when compared to alternative methods like plates and screws, which only achieve about 80% in similar scenarios.
However, every method has its downsides. Plate fixation involves extensive soft tissue dissection, which may lead to complications. Also, it can limit blood supply to the bone. Intramedullary nailing may result in complications such as malunion or nonunion in cases with proximal humeral fractures. These risks suggest that surgeons should carefully evaluate each patient’s fractures.
**Tips**: Always discuss the pros and cons with an orthopedic surgeon. Understanding the specifics can help in choosing the best option. Recovery varies; maintaining a positive mindset is crucial. Regular follow-ups can detect issues early, avoiding potential setbacks in healing.
| Fixation Method | Advantages | Disadvantages | Recovery Time |
|---|---|---|---|
| Humeral Interlocking Nail | Stable fixation, less infection risk, minimally invasive | Requires special equipment, potential for hardware failure | 6-12 weeks |
| Plate Fixation | Good stability, direct bone contact, familiar technique | Higher infection risk, longer incisions | 8-14 weeks |
| Intramedullary Rod | Less tissue disruption, effective for long bones | Limited to specific fractures, may require additional support | 6-10 weeks |
| External Fixation | Versatile, minimizes internal damage, easily adjustable | Cosmetic disadvantages, risk of pin site infections | 8-12 weeks |
Postoperative care is crucial after surgery involving humeral interlocking nails. These specialized nails support bone healing, which is vital for recovery. Studies indicate that proper postoperative rehabilitation can enhance recovery speed by up to 30%. Patients are expected to engage in early mobilization within a few days post-surgery. This can significantly reduce stiffness and improve overall arm functionality.
Pain management is another essential aspect of postoperative care. Many patients experience discomfort after the procedure. Pain control can influence recovery outcomes. Inadequate pain relief might lead to delayed mobility and increased complications. It’s essential to follow recommended pain management protocols. This ensures a smoother recovery and a quicker return to daily activities.
In terms of follow-up, regular check-ups are vital. Monitoring nail position and assessing bone healing is important. Imaging studies are often conducted within six weeks post-surgery. These check-ups help identify any potential issues early. However, some patients may struggle with adherence to follow-up appointments. This can impact overall healing. Addressing these challenges starts with clear communication from healthcare providers.